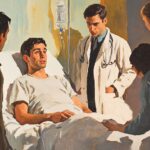
Chemotherapy can increase your risk of developing blood clots, such as deep vein thrombosis (DVT) and pulmonary embolism (PE), which may lead to serious health issues if not recognized and managed early. By understanding the signs, risk factors, and preventive steps, you can work closely with your healthcare team to reduce this risk and stay safer throughout your cancer treatment. This guide will help you know what to look out for, how to prevent clots, and the treatment options available if clots occur.
What Are Blood Clots and Why Do They Happen During Chemotherapy?
Blood clots are gel-like clumps that form when blood thickens and sticks together, potentially blocking the flow through blood vessels. Chemotherapy can increase the likelihood of clot formation by changing blood thickness and the number of blood cells. Certain cancer types—for example, pancreatic and lung cancers—also raise the risk of blood clots.
Your treatment might involve central venous catheters (small tubes placed into large veins for medication delivery), which can sometimes contribute to clot formation. Knowing this connection helps you stay alert to any changes in your body.
Using anticoagulant medications such as warfarin or heparin can help prevent clots by thinning the blood, but these should always be taken under your doctor’s guidance to balance benefits and risks.
Recognizing the Signs and Symptoms of Blood Clots
It’s important to notice warning signs early so you can get help quickly. Common symptoms for DVT include swelling, pain, redness, or warmth in one limb, usually in your leg. Symptoms of pulmonary embolism—a clot that has traveled to the lungs—include sudden difficulty breathing, chest pain, or coughing up blood.
If you experience any of these symptoms, reach out to your healthcare provider immediately. Early detection can prevent more serious complications.
Your Personal Risk Factors for Blood Clots During Chemotherapy
Your risk depends on several individual and treatment-related factors. You may be at higher risk if you:
- Have a personal or family history of blood clots or clotting disorders
- Are undergoing chemotherapy with drugs like cisplatin, gemcitabine, or thalidomide
- Have certain types of cancer, especially pancreatic or lung cancer
- Use central venous catheters for treatment
- Experience reduced mobility during treatment
Discussing these factors with your healthcare team allows them to create a prevention strategy tailored to your needs. For more detail on risk factors, visit the American Cancer Society’s guide on blood clots and cancer.
Preventing Blood Clots: What You Can Do
You play an important role in reducing your clot risk. You can:
- Stay as physically active as possible—simple leg exercises and regular short walks help improve circulation
- Wear compression stockings if recommended by your healthcare provider, especially during long periods of sitting or travel
- Take anticoagulant medications exactly as prescribed
- Stay hydrated and maintain a balanced diet to support overall health
Always talk to your care team before starting any prevention measures, so they can consider your specific treatment and health status. Detailed advice on prevention is available from the Mayo Clinic.
How Are Blood Clots Treated During Chemotherapy?
If a blood clot is detected, your treatment team will usually prescribe anticoagulants to stop the clot from growing and prevent new clots. These medicines include heparin injections or oral drugs like warfarin or newer agents. Regular blood tests help your doctor adjust doses to keep treatment safe and effective.
In some cases, especially with large clots or complications, additional treatments or hospital care may be required. Your healthcare provider will guide the best approach based on your situation.
Follow-Up Care: Staying Vigilant After Chemotherapy
Regular medical check-ups during and after chemotherapy are essential to monitor your health and catch any clot-related problems early. Your healthcare team will do physical exams, blood tests, and imaging if needed to watch for clots or side effects of treatment.
Remember to tell your doctors promptly if you notice symptoms like unexplained limb swelling, pain, or shortness of breath. Staying informed and proactive helps ensure your treatment is as safe as possible.
Frequently Asked Questions
Why does chemotherapy increase my risk of blood clots?
Chemotherapy can change how your blood cells and blood vessels function, making your blood thicker and more likely to form clots. This, combined with some cancer types and treatments, increases your risk of developing clots.
What are the warning signs of a blood clot I should watch for?
Look for swelling, redness, warmth, or pain in your limbs, mostly legs, which may indicate deep vein thrombosis. Sudden breathlessness, chest pain, or coughing up blood could signal a pulmonary embolism—these require immediate medical attention.
Can lifestyle changes really help reduce my risk?
Yes. Staying active, avoiding long periods of sitting, wearing compression stockings if advised, staying hydrated, and avoiding tobacco use can all lower your risk during chemotherapy.
Should I tell my doctors if I have had blood clots before?
Absolutely. Sharing your history of blood clots or clotting disorders is critical so your care team can take extra precautions and monitor you closely during your treatment.
Where can I learn more about managing blood clots during cancer treatment?
Trusted resources include the National Cancer Institute, American Cancer Society, and educational videos from Mayo Clinic’s YouTube channel.