Lymphedema is a chronic condition characterized by the accumulation of lymph fluid in tissues, leading to swelling, often in the limbs. This condition is commonly seen in patients after cancer treatments such as surgery, radiation, or chemotherapy. Understanding lymphedema and its risk factors is crucial for cancer survivors, particularly those with breast cancer, to manage symptoms and improve their quality of life.
Preventing lymphedema involves implementing prevention measures such as:
- Regular exercise
- Maintaining a healthy weight
- Avoiding injuries to the affected area
Techniques such as physical therapy, compression garments, and weight management can significantly reduce the risk. Managing symptoms through compression, exercise, and manual lymphatic drainage is essential for maintaining mobility, reducing tissue fibrosis, and enhancing comfort.
Early detection and treatment of lymphedema are vital. Recognizing symptoms like swelling and skin changes and seeking medical help promptly can prevent complications, such as cellulitis, and enhance health outcomes. Consult healthcare professionals for personalized strategies and support in managing this condition effectively, including evidence-based literature and healthcare recommendations.
Key Takeaways:
Understanding Lymphedema
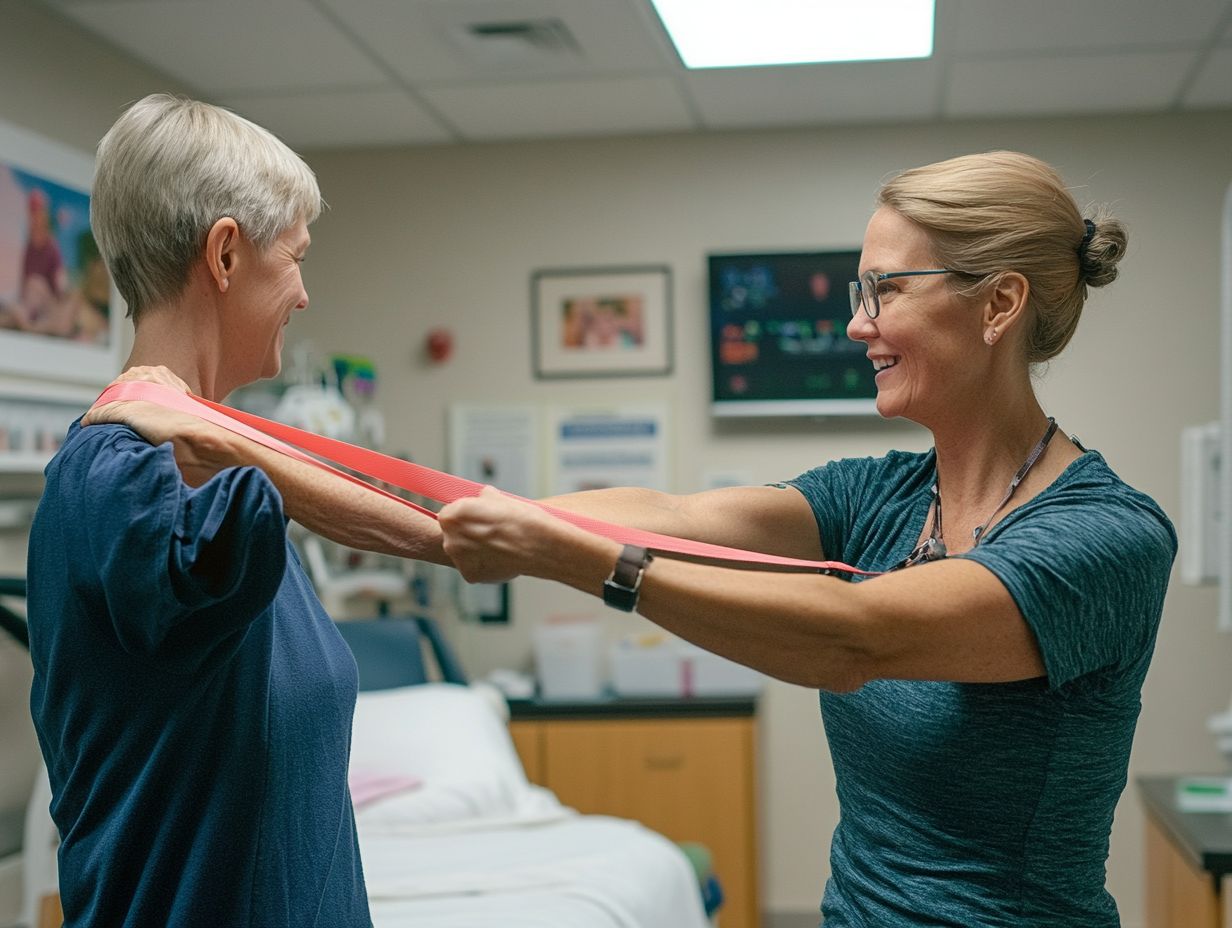
Lymphedema is a chronic condition where lymph fluid accumulates in tissues, causing swelling, often in the limbs.
Lymphedema commonly occurs after cancer treatments like surgery, radiation, or chemotherapy.
Understanding lymphedema is essential for managing symptoms and improving quality of life for affected patients.
What is Lymphedema and How Does it Develop?
Lymphedema is the abnormal accumulation of lymph fluid in tissues, causing swelling in the arms or legs.
Lymphedema develops when the lymphatic system, responsible for fluid balance and immune function, is damaged, often by cancer treatments like surgery or radiation.
Damage to lymph nodes disrupts lymph fluid flow, leading to a build-up in tissues and resulting in swelling, discomfort, and restricted movement.
Risk Factors for Lymphedema After Cancer Surgery
Risk factors for lymphedema after cancer surgery include the type of surgery, such as radical mastectomy or lymph node removal, and lifestyle factors like high body weight and low physical activity levels. Surgical complications, such as damage to lymphatic vessels, can also increase the risk.
Additional risk factors involve infection, injury to the affected area, and radiation therapy, which can exacerbate lymphedema development. Infection prevention is crucial to mitigate these risks.
Identifying Potential Causes
Causes of lymphedema include damage to the lymphatic system during cancer treatments like radiation and surgery, including lymphoscopic interventions and lymphaticovenous anastomosis.
Lymphedema occurs when lymphatic vessels are compromised, reducing fluid transportation capacity and increasing swelling risk.
Monitoring lymphatic function helps detect issues early, allowing interventions such as non-invasive techniques like ultrasound and magnetic resonance imaging to prevent or manage lymphedema.
Preventing Lymphedema

Preventing lymphedema involves regular exercise, maintaining a healthy weight, and avoiding injury to the affected area.
Avoid tight clothing, including tight fitting garments, practice good skin care, and monitor for early signs of swelling to prevent lymphedema.
Consult healthcare professionals for personalized prevention strategies and healthcare strategies that incorporate their expertise and clinical trials.
Strategies for Reducing Risk
Strategies for reducing the risk of lymphedema include:
- Physical therapy, which focuses on therapeutic exercises to enhance lymphatic circulation and improve mobility.
- Weight management, which reduces pressure on the lymphatic system and supports lymph flow.
- Compression garments, which apply pressure to prevent lymph fluid buildup and promote drainage.
Managing Lymphedema Symptoms
Managing lymphedema symptoms involves reducing swelling and discomfort through compression garments, exercise, and manual lymphatic drainage, as well as using lymphatic drainage massage techniques.
Lymphedema management is crucial for cancer survivors to maintain mobility, manage edema, and improve quality of life.
Treatment Options and Coping Mechanisms
Lymphedema treatment includes manual lymphatic drainage, compression wraps, and exercises to reduce swelling, as well as advanced surgical treatments like lymphovenous bypass for severe cases.
Additional options involve skin care routines, pneumatic compression devices, and surgical interventions like lymphovenous anastomosis for severe cases.
Coping mechanisms include education, emotional support, and daily self-care to manage symptoms, alongside pain management strategies.
Importance of Early Detection and Treatment

The importance of early detection and treatment of lymphedema lies in its ability to improve management and enhance patient health outcomes.
Early detection of lymphedema helps initiate timely treatment, reducing symptoms and preventing complications. Regular ultrasound examination and lymphoscintigraphy can aid early diagnosis.
Effective management of lymphedema from an early stage improves quality of life.
Recognizing Symptoms and Seeking Help
Lymphedema symptoms include swelling, discomfort, and changes in skin texture.
Recognizing these symptoms and seeking medical help promptly can prevent complications like infections, improve treatment outcomes, and prevent fluid retention.
Frequently Asked Questions
1. How can I prevent lymphedema after cancer surgery?
There are several ways to help prevent lymphedema after cancer surgery, including avoiding any injury or trauma to the affected area, practicing good skin care, and wearing compression garments.
2. Can exercise help prevent lymphedema after cancer surgery?

Yes, gentle exercise can help improve lymphatic flow and reduce the risk of developing lymphedema after cancer surgery. However, it is important to consult with your doctor or healthcare team before starting any new exercise routine.
3. What should I do if I notice swelling or changes in my affected limb after cancer surgery?
If you notice any changes in your affected limb, such as swelling, heaviness, or tightness, it is important to consult with your doctor as soon as possible. Early detection and treatment can help prevent lymphedema from developing or becoming worse.
4. Are there any dietary changes I should make to prevent lymphedema after cancer surgery?
While there is no specific diet to prevent lymphedema, maintaining a healthy weight and staying hydrated can help reduce your risk. It is also important to avoid extreme temperatures and limit your salt intake, as these can contribute to fluid retention.
5. Can I still receive massages or acupuncture after cancer surgery?
It is important to consult with your doctor before receiving any type of massage or acupuncture on the affected area. Some techniques may be beneficial, while others may increase your risk of developing lymphedema.
6. Is there any medication I can take to prevent lymphedema after cancer surgery?
There is currently no medication specifically designed to prevent lymphedema. However, your doctor may prescribe antibiotics if you have had lymph nodes removed during surgery to reduce your risk of developing an infection, which can lead to lymphedema. Regular blood pressure monitoring may also be advised to avoid exacerbating the condition.





