Hey, if you’re an AYA patient dealing with cancer symptoms at the UC Davis Comprehensive Cancer Center (UCDCCC), sitting in an adult infusion room can feel really lonely amid all those older faces. You’ve probably noticed how tough it is to connect when everyone’s at such different life stages. This piece breaks down the “peer gap” and why it hits so hard, plus what it means for your emotional well-being.
Key Takeaways:
Understanding AYA Patients
AYA patients, or adolescents and young adults typically aged 15-39 as defined by the National Cancer Institute (NCI), face cancer during pivotal life stages, amplifying their unique challenges. These individuals often confront disrupted education and delayed career starts amid chemotherapy sessions that induce fatigue and nausea. Their treatments clash with the demands of building independence, fostering a profound sense of isolation in adult infusion rooms.
Unlike pediatric patients surrounded by playful peers or older adults with established support networks, AYA individuals navigate social milestones like dating and family formation while managing side effects such as pain and vomiting. Research from a study like NCT04594096 suggests these disruptions heighten emotional strain, making peer connections essential for coping. Qualitative analysis of patient interviews reveals recurring themes of loneliness during infusions.
Practical self-management strategies prove vital, including journaling to process unexpected fevers or ER visits that interrupt daily functioning. Curious about [how to handle a cancer diagnosis at a young age](https://www.together4cancer.com/post/how-do-i-handle-a-cancer-diagnosis-at-a-young-age/)? Experts recommend seek AYA-specific oncology guidance to address fertility concerns and access e-health tools for home-based symptom management. This tailored care enhances quality of life amid survival rates uncertainties.
By recognizing these needs, healthcare providers can bridge the peer gap, offering validation through shared experiences. AYA patients benefit from forums where young adults discuss relationships and milestones, countering the isolation of adult settings filled with generational divides.
Defining the AYA Demographic
The National Cancer Institute defines AYA patients as those aged 15-39 diagnosed with cancer, a group with distinct survival challenges. Common diagnoses include leukemia and lymphoma, which demand intensive treatments like chemotherapy in infusion rooms. This age span positions them awkwardly between pediatric and adult oncology services, leaving many without age-appropriate peers.
Adolescents in this demographic miss school events and proms, while young adults postpone career launches or weddings due to treatment demands. Fatigue and nausea from medications often force reliance on family or friends, complicating independent living. Access to specialized care remains limited, exacerbating feelings of isolation.
Experts recommend patients seek AYA-specific resources, such as those provided by the UCLA Health AYA Oncology Program, from the NCI to connect with tailored support networks. These tools aid in navigating side effects like anticipatory vomiting or pain management at home. Such guidance fosters better emotional resilience during prolonged treatments, using remedies like ginger chews or Doterra Serenity oil.
Understanding this demographic highlights the need for oncology programs that integrate peers, reducing the peer gap in adult environments. Interviews from AYA experiences underscore how shared stories improve coping with fevers and unexpected complications.
Unique Psychosocial Needs
AYA patients grapple with disruptions to education, fertility concerns, and social milestones that older adults have often already passed. Peer relationships become crucial for discussing dating dilemmas or career advice absent in mixed-age infusion rooms. This isolation intensifies emotional distress amid ongoing chemotherapy.
Fatigue and nausea hinder daily functioning, prompting many to journal emotions for self-management. Online AYA forums provide validation through stories of self-management of pain or vomiting without judgment. These social spaces help young adults process loneliness during treatments.
- Join virtual support groups for adolescents facing similar side effects.
- Explore e-health apps for tracking symptoms like fever at home.
- Seek guidance from oncology teams on fertility preservation before therapy starts.
Such steps build resilience, addressing the peer gap effectively, as shown in experiences from the Netherlands Cancer Institute using tools like MOS-SSS and EORTC CAT.
Qualitative analysis of patient experiences emphasizes relationships with peers who understand milestones like starting a family. Practical remedies, from medications to peer-shared tips, enhance quality of life and reduce ER visits for unmanaged symptoms like unexpected fever, even during COVID-19.
The Adult Infusion Room Environment
Adult infusion rooms, where chemotherapy and other treatments occur, are typically filled with older patients, creating an environment misaligned with AYA experiences. These spaces feature rows of recliners under fluorescent lights, with nurses monitoring side effects like nausea and fatigue. Young adults and adolescents often feel out of place amid the subdued tones and familiar routines.
The setting emphasizes medical efficiency, with beeping monitors and the scent of antiseptics dominating the air. AYA patients, navigating cancer amid life milestones, crave social connections absent here. This mismatch heightens emotional isolation during long sessions.
Routines focus on treatment administration and symptom management, yet lack peer support tailored to younger needs. Bringing personal items helps bridge the gap. Experts recommend seeking oncology guidance to adapt these environments for better quality of life.
Observations from patient interviews reveal how such rooms amplify loneliness for AYA individuals. Qualitative analysis of experiences underscores the need for age-specific care. Integrating e-health tools can foster relationships beyond the room.
Patient Demographics and Age Dynamics
Most patients in adult infusion rooms are over 50, leading to interactions dominated by retirement stories rather than the school or job concerns of younger individuals. AYA patients, facing cancer during formative years, encounter generational storytelling gaps. This dynamic triggers personal isolation, as discussions rarely touch on peers or young adult challenges.
Observing room dynamics reveals subtle cues, like shared anecdotes about grandchildren versus milestones with friends. Adolescents and young adults feel sidelined, exacerbating emotional strain from fatigue and pain. Such mismatches hinder social support vital for self-management.
Research suggests fostering peer relationships counters this age divide. AYA individuals benefit from noting triggers, such as overheard conversations on past careers, to mentally distance themselves. Seeking specialized oncology programs can align care with their unique experiences.
Interviews highlight how demographic contrasts intensify loneliness during treatments. Experts recommend observing these patterns to understand isolation roots. Building external networks aids emotional functioning amid survival challenges.
Daily Atmosphere and Routines
Infusion days involve hours of waiting with fixed seating, hushed conversations, and shared magazines geared toward older interests. Pre-treatment check-ins assess symptoms like vomiting and fever, followed by lengthy chemotherapy drips. AYA patients often personalize spaces with headphones to escape the unfamiliar rhythm.
Routines include regular side effect monitoring, with nurses addressing anticipatory nausea or unexpected pain via medications. The atmosphere remains clinical, limiting casual bonds over shared young adult struggles. Bringing books or e-health devices supports self-management and home-like comfort.
Practical personalization tips ease the day: pack noise-canceling headphones for privacy, select engaging reads on functioning through cancer, and use apps for peer connections. These steps mitigate isolation during monitoring intervals. Guidance from medical teams enhances remedy access.
Qualitative experiences show routines amplify peer gaps for AYA, impacting quality of life. Families and friends can assist by coordinating visits. Proactive management of fatigue and ER risks preserves emotional well-being.
Core Causes of the Peer Gap
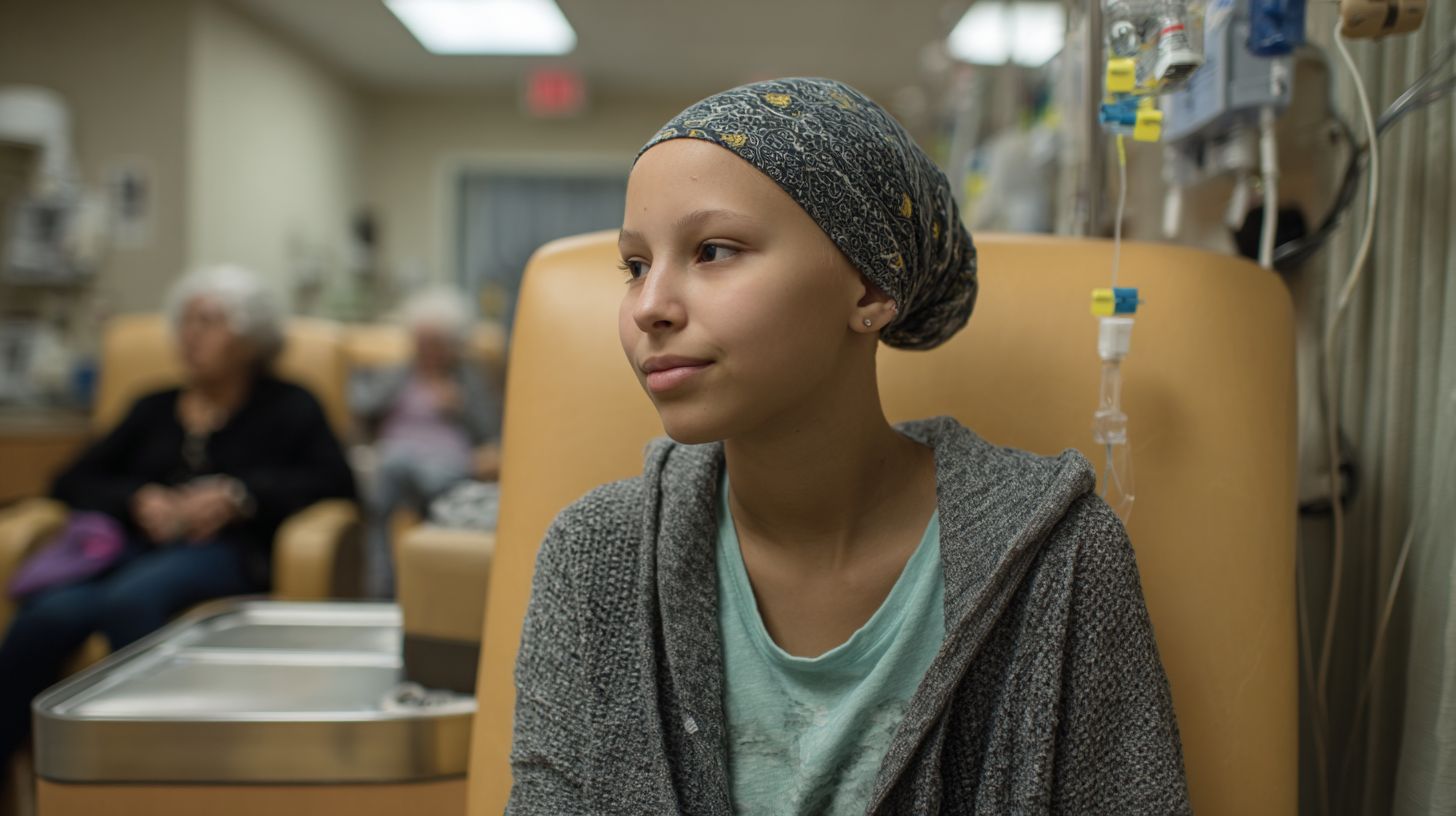
The peer gap stems from fundamental mismatches in communication styles and life experiences between AYA patients and their older peers. In adult infusion rooms, where chemotherapy sessions unfold amid shared vulnerability, adolescents and young adults (AYA) often feel isolated. This disconnect amplifies emotional loneliness, hindering the social support essential for managing side effects like fatigue and nausea.
Root causes trace to generational divides that shape interactions during treatment. Older patients, shaped by different eras, gravitate toward narratives of family legacies, while AYA individuals seek concise, digital exchanges. Such mismatches disrupt rapport, leaving young adults adrift in oncology settings designed for broader age groups.
Experts recommend fostering shared treatment realities to bridge these divides, as measured by tools like MOS-SSS or EORTC CAT. By focusing on common challenges like pain management or anticipatory vomiting, patients can cultivate connections beyond demographics. Qualitative interviews reveal that intentional efforts reduce isolation, enhancing quality of life amid cancer care.
Addressing these core causes enables AYA patients to seek peers who understand their unique position. To discover online communities tailored for cancer care, young adults can bridge the peer gap through digital connections that match their communication preferences. This shift promotes self-management strategies and emotional resilience, vital for navigating milestones disrupted by therapy.
Generational Communication Barriers
Baby boomers may discuss family histories while AYA patients prefer quick texts or memes, hindering natural rapport. This clash in communication styles creates awkward silences during long infusion sessions. Young adults, comfortable with e-health tools for symptom tracking, find traditional storytelling unrelatable.
Slang differences exacerbate the divide; terms like “lit” for positive vibes puzzle older peers, while dated phrases confuse AYA patients. Tech comfort levels vary widely, with younger ones relying on apps for nausea remedies or fever alerts, unlike elders’ preference for verbal exchanges. Such barriers foster social isolation in shared spaces.
To bridge gaps, try icebreaker questions about hobbies or favorite shows. Ask, “What music helps you through treatment?” or “Any apps you use for fatigue management?” These open doors to mutual understanding without forcing generational alignment.
Practical guidance includes modeling concise sharing, like texting memes about unexpected side effects. Over time, these efforts build relationships, offering emotional support akin to peers at home or with friends.
Differing Life Stage Experiences
While older patients share grandchild stories, AYA individuals miss weddings, graduations, or first jobs due to cancer treatment. This life stage contrast underscores profound disparities in adult infusion rooms. Young adults grapple with fertility fears during chemotherapy, distinct from post-menopause discussions among elders.
AYA patients navigate disrupted milestones, like delayed career starts amid vomiting or ER visits for fever. Older peers, often post-family-building, focus on legacy tales that highlight survival rates and long-term functioning. These narratives, though inspiring, sideline the acute emotional isolation young adults feel.
Find common ground by emphasizing shared treatment realities, such as coordinating medications for pain or self-management of side effects. Discuss practical tips like home remedies for nausea, creating bonds over universal cancer experiences rather than divergent paths.
Experts recommend steering conversations toward oncology-specific challenges, like balancing care with social relationships. This approach validates AYA struggles, fostering support networks that enhance quality of life and reduce loneliness in clinical settings.
Emotional and Psychological Impacts
The peer gap intensifies feelings of otherness, exacerbating emotional strain during already vulnerable treatment phases. AYA patients undergoing chemotherapy often grapple with profound loneliness amid older peers discussing retirement or grandchildren. This disconnect heightens emotional isolation, making infusions feel like solitary ordeals.
Such experiences disrupt daily functioning and quality of life, as young adults miss shared stories about career milestones or family life, sometimes compounded by COVID-19 restrictions. Symptoms like fatigue and nausea compound the burden, turning treatment rooms into spaces of unspoken fears. Practical self-management through mindfulness apps tailored for cancer patients offers relief, guiding users through breathing exercises amid infusions.
Experts recommend integrating these tools with journaling to process anticipatory anxiety before sessions. Over time, this builds resilience against unexpected side effects like pain or fever. Seeking oncology social support early fosters long-term emotional health.
Qualitative analysis of patient interviews reveals how virtual e-health connections bridge gaps, easing the path to survival and thriving post-treatment. These strategies enable AYA individuals to reclaim agency in their care journey.
Feelings of Isolation and Invisibility
Many AYA patients describe sitting silently amid older chatter, feeling like outliers in their own treatment space. The hum of conversations about decades-past diagnoses underscores their unique position as young adults facing cancer. This loneliness during long infusion hours amplifies a sense of invisibility.
Relatable scenarios emerge, such as watching peers swap tips on managing vomiting or medications while one’s own concerns about fertility or relationships go unvoiced. Pre-planning peer calls before sessions counters this, providing timely emotional anchors from home. Such preparation transforms passive waiting into active connection.
Using apps like the AYA Match app for virtual peer connections links adolescents and young adults with shared experiences of side effects and milestones. These platforms facilitate quick chats about fatigue or ER visits, reducing isolation. Regular engagement builds lasting social support networks.
Over sessions, patients report improved quality of life, as these remedies validate their distinct journeys through treatment.
Heightened Anxiety and Depression
Lack of peer understanding can amplify worries about side effects from drugs like Doxorubicin, Cytarabine, Daunorubicin, Methotrexate, Vincristine, or trials like NCT04594096, deepening mental health struggles. AYA patients often cycle through unshared fears of how chemotherapy impacts relationships or career goals, unlike older counterparts with different life stages. This mismatch fuels anxiety and depressive episodes.
Unexpected symptoms like nausea or pain trigger spirals, especially without relatable stories to normalize them. Seeking oncology social support breaks this pattern; start by requesting group therapy referrals from medical teams. These sessions offer safe spaces to unpack emotional burdens.
Practical steps include:
- Discussing fears openly with care providers during check-ins.
- Joining AYA-specific support groups for tailored guidance.
- Tracking moods via apps to identify depression triggers early.
Integrating these with self-management techniques enhances emotional resilience, aiding access to peers and improving overall functioning amid treatment challenges.
Communication Challenges
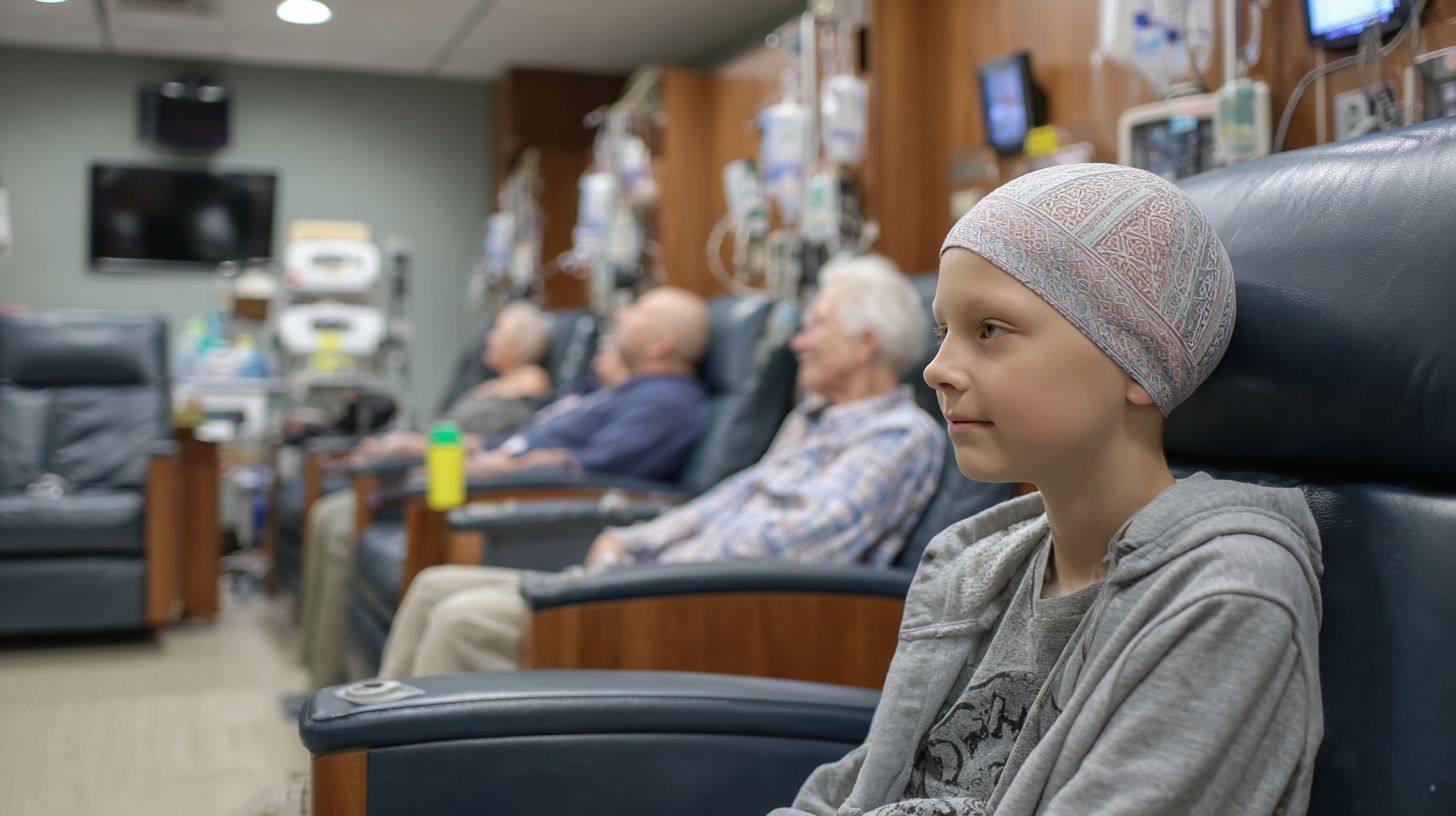
Age differences stifle open sharing, leaving AYA patients without the relatable support vital during chemotherapy. In adult infusion rooms, older patients often discuss chronic pain management or family legacies, while young adults grapple with disrupted milestones like careers and relationships. This mismatch fosters emotional isolation, hindering the peer validation essential for coping with side effects such as fatigue and nausea.
Qualitative analysis of patient experiences reveals how generational divides limit discussions on fertility concerns or social anxieties. Adolescents and young adults hesitate to voice fears of anticipatory nausea or unexpected vomiting amid talks of retirement. Bridging this requires gentle prompts to foster inclusive dialogue.
Experts recommend oncology teams facilitate structured sharing sessions tailored to diverse needs. Such approaches enhance quality of life by addressing both physical symptoms like fever prompting ER visits and emotional hurdles. Patients gain tools for self-management, reducing loneliness in treatment settings.
Encouraging cross-age empathy through shared stories of cancer survival can transform infusion rooms into supportive spaces. AYA individuals benefit from guidance on navigating relationships and home functioning amid therapy. This communication shift promotes access to holistic care.
Reluctance to Share Among Age Groups
Younger patients hesitate to voice dating woes or body image fears to those focused on aches and pensions. This self-censorship stems from perceived irrelevance, leaving AYA individuals isolated during infusions. Older peers, immersed in their own symptom management, rarely relate to fertility pauses or career disruptions.
In these settings, discussions often center on medications for pain or long-term functioning, sidelining unique AYA struggles like social withdrawal from nausea. Patients withhold stories of missed milestones with friends and family, deepening emotional gaps. Gentle interventions can encourage openness without discomfort.
Try this script: Treatment affects my social life-how about yours?
It invites reciprocity while highlighting shared impacts on quality of life. Another option: I’ve been dealing with body image changes from chemo-anyone else?
These prompts build mutual understanding, easing reluctance across ages.
Oncology guidance emphasizes practicing such phrases to overcome barriers. Regular use fosters peer connections, aiding self-management of side effects like fatigue. AYA patients report less loneliness when sharing experiences freely in group dynamics.
Lack of Relatable Peer Support
Without peers facing similar fertility or career pauses, AYA patients miss validation for their specific struggles. Adult rooms lack empathy for young adult challenges like maintaining relationships amid chemotherapy. This void amplifies feelings of isolation during treatment for cancer symptoms.
Older patients offer wisdom on enduring pain or vomiting, yet overlook adolescent-specific concerns such as school disruptions or future family planning. AYA individuals crave discussions on emotional self-management and home functioning. Absent targeted support, they navigate side effects like fever alone.
Seek connections through Childrens Oncology Group networks, which link adolescents and young adults for shared experiences. E-health platforms provide virtual spaces to discuss nausea remedies or survival anxieties with relatable peers. These resources deliver the empathy missing in traditional infusion environments.
Experts recommend prioritizing such outlets for quality-of-life gains. Interviews with AYA patients underscore how peer validation eases loneliness and boosts access to practical advice on medications. Building these ties transforms isolation into communal strength during oncology care.
Structural and Logistical Issues
Beyond social factors, physical room designs and schedules reinforce separation among patients. Adult infusion rooms often prioritize efficiency over peer interactions, leaving adolescents and young adults (AYA) with cancer feeling isolated during chemotherapy. These facility-based problems exacerbate emotional loneliness and hinder access to relatable support.
Rigid layouts and fixed timetables limit opportunities for AYA patients to connect with peers facing similar side effects like fatigue and nausea. Structural barriers disrupt daily functioning, pulling young adults away from work or school while stranding them amid older crowds. Experts recommend targeted adjustments to foster a sense of community in oncology care.
Practical changes, such as dedicated pods or flexible seating, can improve quality of life for AYA individuals navigating treatment milestones. Qualitative interviews reveal how these issues amplify self-management challenges during infusions. Addressing them promotes better emotional relationships and reduces unexpected ER visits from unmanaged symptoms like fever or pain.
Infusion centers hold the key to bridging this peer gap, enhancing survival experiences through inclusive designs. Guidance from medical teams can guide patients toward advocating for such shifts, easing the burden of isolation in adult-dominated spaces.
Fixed Seating and Social Clustering
Rigid chair assignments group older patients together, stranding AYA individuals on the periphery. This social clustering in infusion rooms intensifies feelings of isolation for young adults enduring chemotherapy side effects like vomiting and anticipatory nausea. Peers become distant, complicating emotional support during long sessions.
Older patients often form tight-knit groups, sharing stories of family and long-term care that differ from AYA experiences. Adolescents feel sidelined, their concerns about milestones and relationships overlooked amid the chatter. Such dynamics heighten loneliness, impacting home functioning and overall well-being.
To counter this, politely request seat switches from staff, positioning yourself near fellow young adults. Bring portable activities like e-health apps, card games, or journals to spark outreach and conversations about shared symptoms such as pain management or fatigue remedies. These steps build tentative connections without disrupting others.
Over time, consistent efforts can transform peripheral spots into hubs of peer support, easing the qualitative burden of cancer treatment. Medical guidance encourages such proactive measures, fostering relationships that extend beyond the infusion room.
Inflexible Scheduling Conflicts
School or work-tied appointments clash with adult-heavy slots, limiting AYA attendance overlap. This mismatch in infusion schedules deepens the peer gap, as young adults miss chances to bond over common challenges like medications and self-management strategies. Isolation persists, amplifying emotional strain during treatment.
Adult patients dominate daytime hours, leaving evenings sparse for AYA crowds juggling education or jobs. Conflicts arise when nausea or fatigue from chemotherapy disrupts routines, forcing suboptimal timing. Research suggests these patterns contribute to poorer quality of life and heightened loneliness.
Advocate for flexible infusion times by discussing needs with your oncology team, highlighting school or work demands. Request evening teen or young adult pods to align schedules and enable peer interactions focused on remedies for side effects like unexpected vomiting or fever. Such adjustments improve access to relatable support.
Persistent advocacy can lead centers to pilot AYA-specific slots, enhancing survival experiences through better social connections. Friends and family benefit too, as reduced isolation aids overall functioning and emotional health in cancer care.
Long-Term Consequences
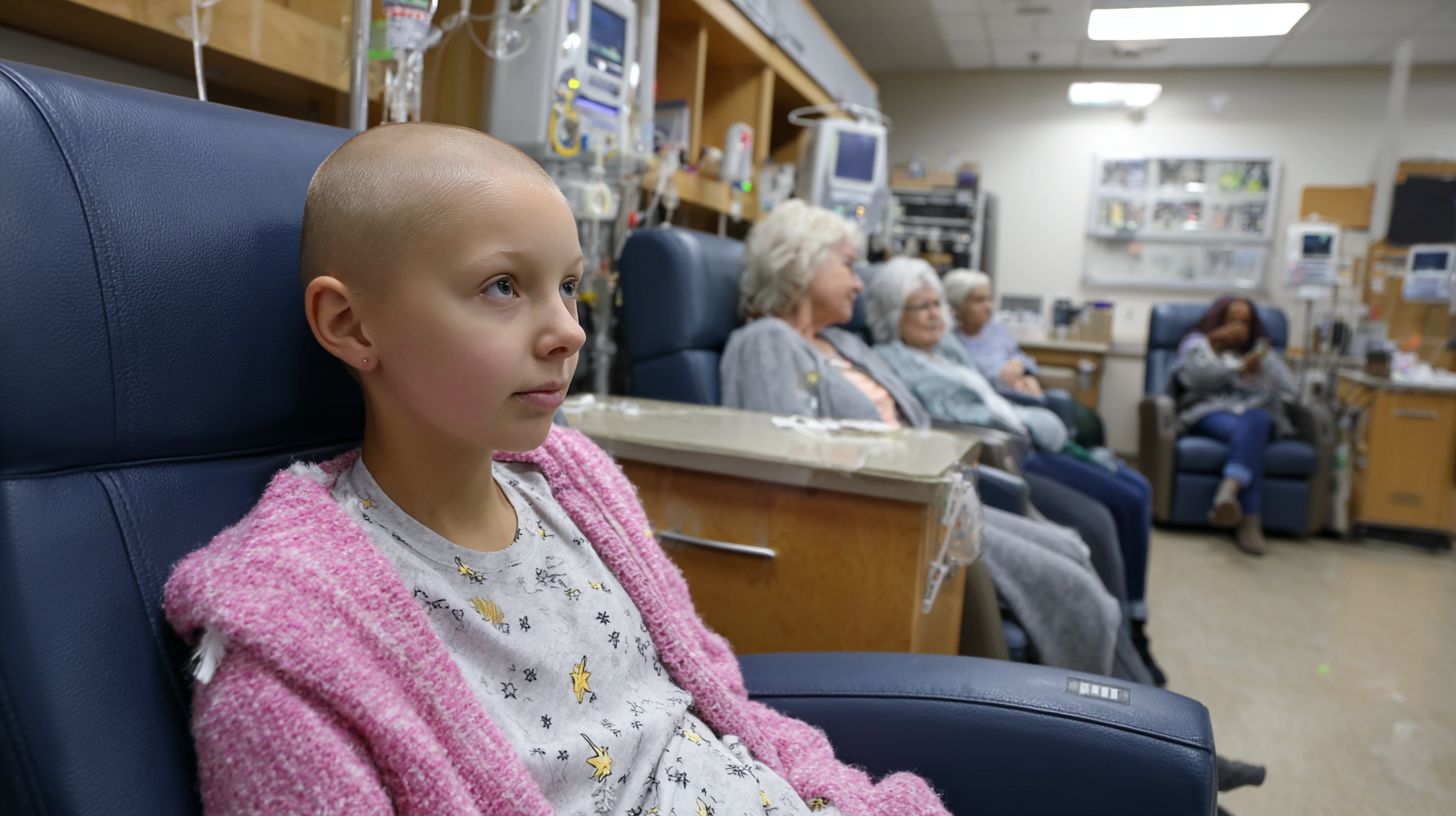
Persistent isolation influences not just daily moods but ongoing health behaviors and well-being. Adolescent and young adult (AYA) patients in adult infusion rooms often face a peer gap that lingers beyond chemotherapy sessions. This disconnection fosters emotional fatigue, altering how they manage side effects like nausea and pain over time.
Without peers who share similar cancer experiences, young adults may neglect self-management strategies at home. Research suggests this leads to poorer treatment adherence and strained family dynamics. Over months or years, such patterns erode overall survival prospects and quality of life.
Experts recommend seeking social support through e-health platforms or oncology groups tailored for AYA. Building connections combats loneliness during milestones like graduations or careers. Proactive steps early on can mitigate these enduring impacts on emotional resilience.
Qualitative analysis of patient interviews reveals how isolation hampers access to guidance on unexpected symptoms such as fever or vomiting. This underscores the need for medical teams to address the peer void in adult settings. Long-term, fostering peer networks enhances functioning and care continuity.
Reduced Treatment Adherence
Feeling unsupported can lead to skipped appointments or delayed side effect reporting amid emotional fatigue. AYA patients, surrounded by older adults in infusion rooms, often ignore nausea or pain during chemotherapy. This stems from lacking peers to normalize such symptoms.
Without shared stories, young adults might skip medications or remedies for vomiting at home. Friends and family provide reminders, yet they cannot fully grasp the cancer journey. Over time, this isolation breeds anticipatory dread, worsening adherence.
To counter this, build accountability systems with family check-ins for symptom logs. Oncology guidance encourages pairing with AYA support groups for motivation. Consistent tracking prevents ER visits from unmanaged fever or severe side effects.
- Set daily reminders for nausea management via apps.
- Share treatment updates with trusted peers online.
- Discuss adherence barriers openly with medical teams.
Impact on Quality of Life
Ongoing disconnection hampers social functioning and emotional resilience long after treatment ends. AYA cancer survivors miss peer bonds that affirm their unique experiences in adult settings. This fosters lasting loneliness amid life’s milestones.
Strained relationships with family and friends emerge as patients withdraw from social circles. Fatigue from isolation compounds challenges in returning to work or school. Quality of life suffers without outlets for discussing chemotherapy’s toll.
Experts recommend daily journals to track emotional and physical shifts. Simple entries on symptoms, joys, and support needs reveal patterns. Pair this with e-health communities for AYA to rebuild connections.
Qualitative studies highlight how peer access improves self-management and well-being. Seeking oncology programs focused on young adults restores functioning. Over time, these steps enhance life satisfaction post-treatment.
Pathways Forward
Targeted interventions can bridge the peer gap, enhancing support for AYA patients in oncology settings. These approaches foster social connections amid chemotherapy and side effects like fatigue and nausea. Practical steps enable young adults to seek age-appropriate care and build relationships.
Options range from dedicated infusion spaces to digital mentorship, addressing emotional isolation during treatment. Patients report improved quality of life through peer interactions that normalize experiences like pain management and milestones missed at home. Experts recommend starting with local research for accessible programs.
Virtual platforms extend support beyond physical rooms, aiding self-management of symptoms such as vomiting and fever. Families and friends benefit too, as AYA patients share guidance on navigating ER visits and medications. These pathways promote resilience and better functioning in daily life.
Qualitative interviews highlight how peer access reduces loneliness, with e-health tools facilitating connections. Survival rates improve indirectly through sustained emotional support during adolescence and young adulthood. Oncology teams play a key role in guiding patients toward these resources.
Age-Segregated Infusion Options
Centers like UC Davis Comprehensive Cancer Center (UCDCCC), the National Cancer Institute (NCI), or the Childrens Oncology Group offer dedicated AYA infusion spaces for peer camaraderie. These environments allow young adults to connect during chemotherapy sessions, easing isolation from older patients. Shared experiences with side effects like nausea build vital support networks.
Models from the Netherlands Cancer Institute inspire similar setups worldwide. Patients discuss remedies for fatigue, pain, and anticipatory symptoms in a relatable setting. This setup enhances quality of life by aligning treatment with social needs.
To access these options, follow these steps:
- Research local options using oncology directories or medical teams, a process taking about 10 minutes.
- Request a transfer through your care provider, emphasizing peer support benefits.
- Avoid assuming availability; confirm details directly to manage expectations.
Such spaces reduce unexpected ER trips from unmanaged symptoms and foster relationships. AYA patients gain confidence in self-management, supported by peers facing similar cancer challenges.
Peer Mentorship Programs
Programs like the AYA Match app connect patients for shared experiences beyond the infusion room. These platforms pair young adults navigating chemotherapy, addressing emotional loneliness through guided conversations. Peers offer insights on managing nausea, fatigue, and family dynamics.
National groups and hospital-based initiatives provide structured mentorship. Participants exchange tips on medications, home remedies, and maintaining functioning amid treatment. This support proves invaluable during vulnerable milestones in adolescence and young adulthood.
Getting started is straightforward with these steps:
- Download a reputable app focused on AYA oncology support.
- Complete your profile in about 15 minutes, noting symptoms and experiences.
- Schedule virtual meets to build connections quickly.
A common mistake is waiting for perfect matches, which delays relief. Instead, embrace initial chats to combat isolation. Research suggests these programs improve access to guidance, enhancing overall care and survival through community.